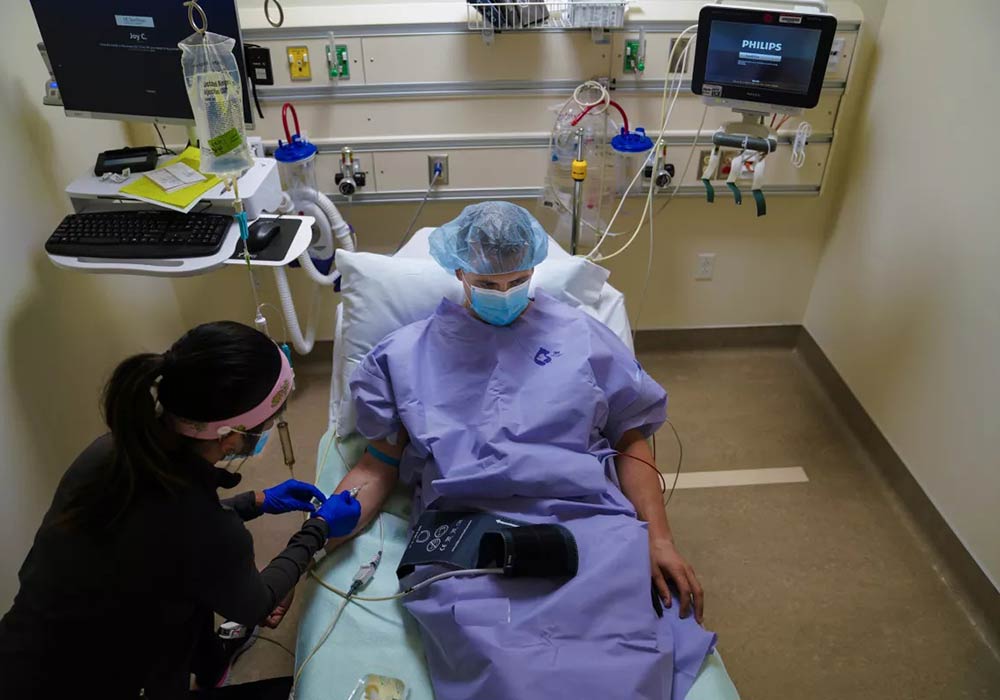
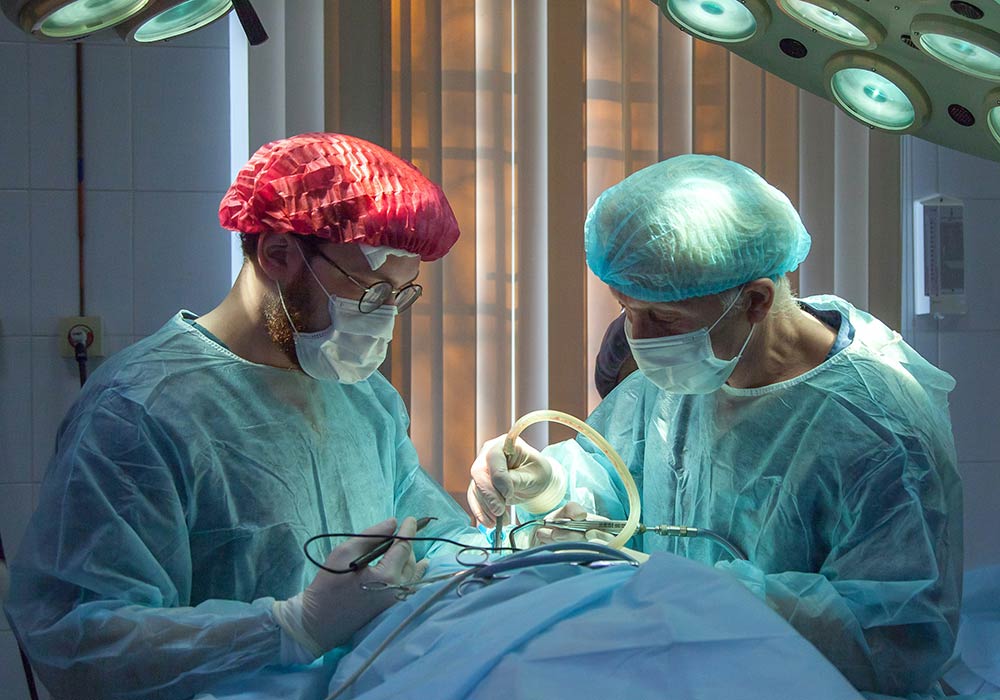
When things go wrong in healthcare, accountability from medical providers and institutions is hard to find. While excellence does exist, it often feels like the exception rather than the standard of care.
In a recent Op/Ed for the Gazette-Times (available here as a PDF), I outline the difficulties Phil encountered when obtaining care for a severed quadricep tendon – a lack of transparency, a failure to listen, and poor communication. Phil’s experience resonates because these are common issues in healthcare today.
Many thanks to the Gazette-Times for publishing this Op-Ed highlighting issues with accountability in healthcare. Read more about the additional obstacles Phil faced when seeking accountability: