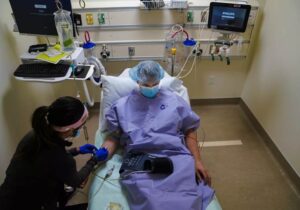
Among the many changes to our lives imposed by the pandemic, one potentially positive offering is on-line doctor appointments. Such visits are variously called: virtual health, telemedicine, telehealth, or virtual care. The patient connects over the internet either through a computer, tablet, or mobile phone rather than meeting with a doctor in the office.
At first glance, there’s great appeal to this option. Virtual meetings eliminate drive times, parking hassles, and long stints in crowded waiting rooms. The neurologist monitoring my multiple sclerosis is based in Portland, an hour and a half drive, one-way, on a crowded interstate. Her office is in a very large and busy medical center, not a place I want to spend any time during a pandemic.
Some Pluses and Minuses of Telemedicine
The feedback on telemedicine from patients and physicians in social media and healthcare literature is mixed. Some patients feel communication with physicians has improved with on–line visits citing more personal interactions and longer appointments. Many patients with chronic conditions are particularly enthusiastic with virtual options. Such patients may experience issues with limited mobility or a desire to limit in-person interactions during Covid-19.
The significant downside of telemedicine is the technology. Not everyone has access to high speed internet, particularly patients that live in rural areas. And the costs associated with purchasing high speed internet is another barrier to access.
My First Telemedicine Visit
As a new patient, my first meeting with the neurologist in Portland occurred at the end of 2019. Due to Covid, our spring appointment moved on-line. I was somewhat nervous about this initial virtual visit.
The logistics of the technology was certainly manageable, just a bit intimidating. I was ecstatic not to have to make the hour and a half drive and to avoid the exposure to other people. Given this was only the second appointment, I was also hopeful that we might be able to advance the relationship in some small way.
In the end, I found the telemedicine interaction disappointing. The visit, while efficient, lacked a personal connection and our time felt abbreviated. More importantly – the appointment was incomplete. Virtual connections are left wanting by their very definition. There is no physical exam, no opportunity for a physician to palpitate, probe, and measure the physical well-being of the patient. (More discussion on the importance of touch in an upcoming post.)
What is Missing…
Here are some of the hands-on measurements that typically occur at each of my in-person neurological appointments:
- Blood pressure
- Eye exam: In a darkened room, the physician shines a small flashlight into each eye. This light reflex test can detect potential nerve damage.
- Nine-hold peg challenge: Using only one hand, I insert nine pegs into small holes on a wooden board and then must remove each of the pegs individually. This is a timed test and measures finger dexterity and eye-hand coordination both indicators of any neurological complications.
- 10-metre walk test: I must walk as quickly as possible to a mark 10-metres from my starting position. This is also a timed test and measures comfort and gait speed.
- Reflex tests: A reflex hammer tapped on my tendons tests whether the reflex response is stronger than normal or more frequent.
- Babinski Sign: The physician scrapes a sharp blunt object along the bottom of the foot. In MS patients the big toe moves up and the toes fan out. Infants have this neurological reflex but then it disappears. When this reflex is present in adults, it is an indicator for MS.
- Pin pricks: A sharp object such as a pin pricked on different points of my feet, legs, hands, and arms tests the integrity of the nerve fibers.
- Tuning fork: A vibrating tuning fork is placed on different points of my feet and I must report when I can no longer feel the vibration.
… And Why it Matters
NONE of these assessments happen in an on-line visit with a doctor. While each of these tests are important to the initial diagnosis of MS they also provide insights for physicians when monitoring the progression of disease. Measuring change has tremendous value since nerve damage can occur that is not always apparent to the patient.
For the past few years, I have noticed a difference in my ability to feel pin pricks and to accurately tell when the tuning fork stops vibrating. When the phrase Babinski Sign showed up on the notes after one of my routine visits, I had to look up what it might mean.
Virtual Care Does Not Replace In-Person Visits
Overall, I am extraordinarily fortunate. My MS has remained stable with few physical manifestations since I was diagnosed in 1993. For patients where MS is more active, physician monitoring and management of the disease is crucial. And the need for regular physical examinations extends across multiple disease states – cardiac health, cancer, diabetes, and other neurological conditions such as ALS and Parkinson’s Disease to name a few.
Pronouncements heralding virtual care as here to stay and the future of medicine are premature. Such visits are a great convenience but should only serve to complement not replace in-person care and treatment. The physician-patient face-to-face meeting is a hallmark of quality healthcare and physical exams are an essential component.
I look forward to the day when I can safely meet with my neurologist in person.
So, tell me – what are your experiences with on-line doctor visits? – I’m very curious to hear how it is going for you.